For HIV-positive patients, anti-retroviral therapy is recommended after a duration of 2-10 weeks after initiation of the anti-fungal therapy. Another crucial aspect of the management of cryptococcosis includes improving the immune status of the patient. Use of medications such as acetazolamide, mannitol and dexamethasone which normally used in bacterial meningitis for lowering intracranial pressure is not recommended in cryptococcal meningitis. Lumbar puncture is the recommended option for management of intracranial pressure and either a ventricular drain or ventriculo peritoneal shunt is used in patients who require frequent lumbar punctures. Monitoring intracranial pressure and keeping it under check plays an important role in reducing the mortality associated with cryptococcal meningitis. Maintenance therapy can be discontinued if the patient achieves a healthy immune status clinically correlated as CD4 cell count of more than 100 cells/microL. Maintenance therapy is recommended with fluconazole after eight weeks of induction and consolidation phases and the duration of maintenance phase is generally for a period of 1 year. After 2 weeks of induction therapy a repeat examination of cerebrospinal fluid is recommended and the duration of induction therapy can further be extended if the cultures remain positive. The medication choices are usually similar in HIV-positive patients, patients with organ transplantation and patients suffering from other conditions that cause immune suppression. Amphotericin B and flucytosine, for a minimum duration of 2 weeks are recommended antifungal therapies that are used for induction phase and fluconazole for a duration of eight weeks is the recommended drug for consolidation phase of the therapy. Antifungal therapy that targets Cryptococcus comprises induction, consolidation, and maintenance phase. Management of CNS cryptococcosis and in immune-compromised hosts involves treatment targeting the fungal pathogen, reducing the intracranial pressure, and improvising the immune status of the patient. In non-immunocompromised patients, a lumbar puncture should be considered ruling out asymptomatic CNS involvement, but the guidelines state that an LP can be avoided in asymptomatic, immunocompetent patients with no CNS symptoms. This is also the treatment recommendation for non-meningeal, non-pulmonary cryptococcosis in patients where CNS disease was ruled out. Per the 2010 IDSA Guidelines, non-immunosuppressive patients suspected of having a pulmonary cryptococcal infection with mild-to-moderate symptoms can be treated with fluconazole at a dose of 400mg daily for 6-12 months. Pharmacological treatment for cryptococcal infections depends on the site of infection and the severity of symptoms. Disseminated infection is commonly associated with HIV infection or several other immunocompromised states. ĭisseminated Cryptococcus infection is defined by a positive blood culture or a positive culture from at least two different sites. 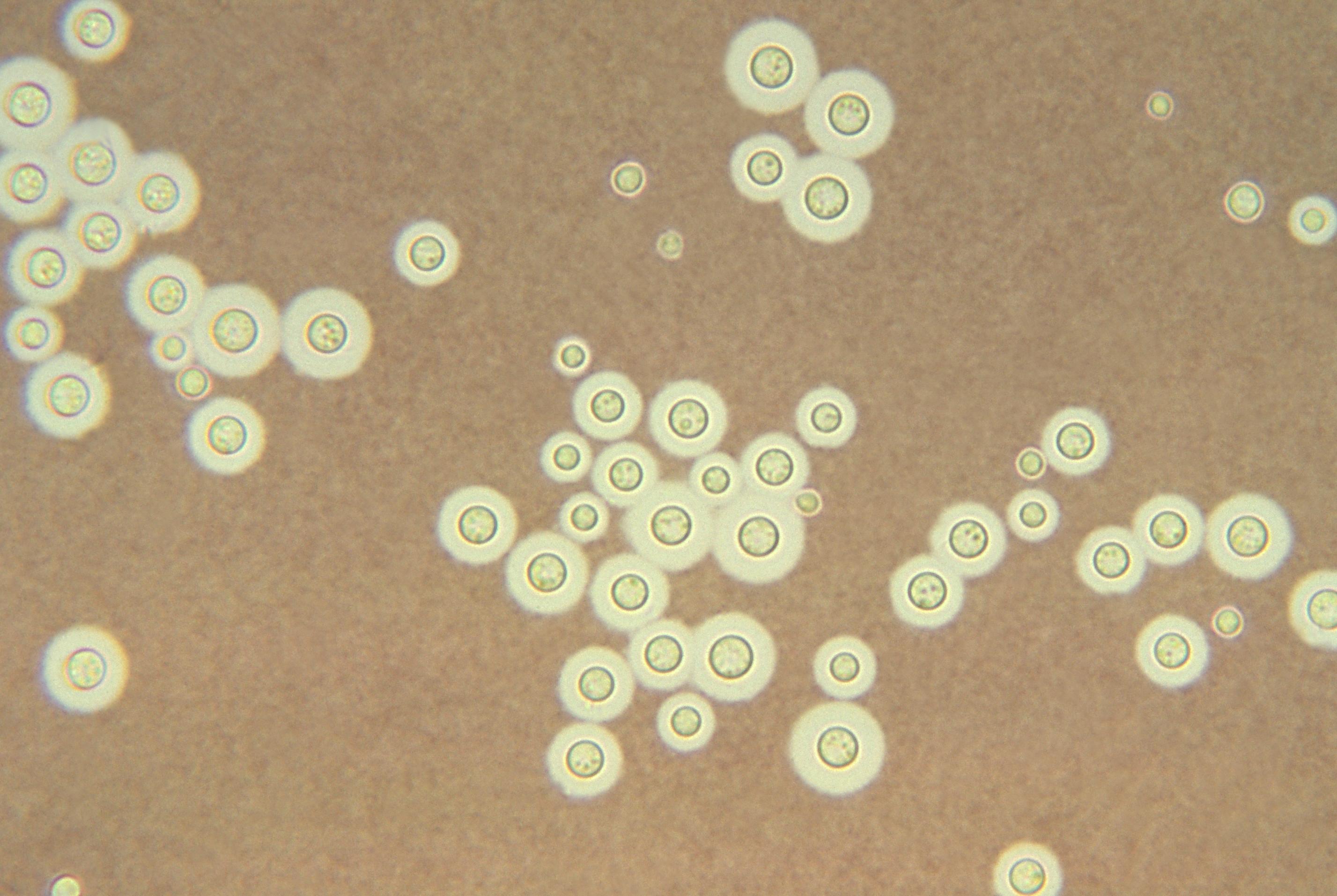
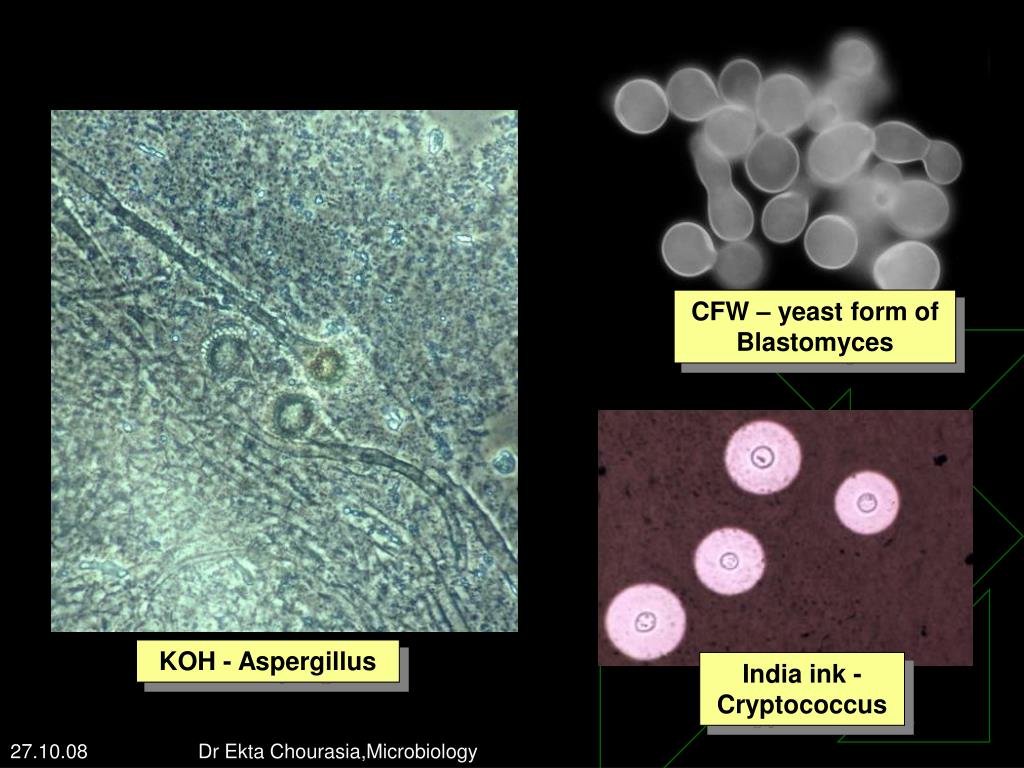
Different techniques such as latex agglutination, enzyme-linked immunosorbent assay (ELISA) and lateral flow assay can be used to confirm the diagnosis of cryptococcal antigen. Detection of cryptococcal antigen through immunodiagnostic tests of the serum and the cerebrospinal fluid provide a definitive diagnosis of the infection. The culture of the infected fluid reveals cream colored colonies in about 3-7 days while staining with Indian ink helps in identifying the organism rapidly. Analysis of the fluid usually shows low white blood cell count, low glucose, and elevated protein but could also be normal in approximately 25-30% of the cases. Cerebrospinal fluid analysis, culture, staining and immunodiagnostic tests of cerebrospinal fluid are the primary diagnostic tests that are performed to diagnose meningitis caused by Cryptococcus. Patients presenting with symptoms of central nervous system are evaluated with radiographic imaging of the brain to rule out the presence of elevated cerebrospinal fluid pressure. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
